What Is a Tilt Table Test, and What Does It Tell You?
A tilt table test is a specialized autonomic nervous system evaluation used to measure how your body regulates blood pressure, heart rate, and circulation when changing from a lying position to standing upright. The test is commonly used to diagnose conditions such as postural orthostatic tachycardia syndrome (POTS), orthostatic hypotension, vasovagal syncope, and other forms of dysautonomia.
For many patients experiencing dizziness, fainting, rapid heart rate, fatigue, brain fog, or exercise intolerance, the tilt table test provides important insight into how the nervous system responds to gravity and orthostatic stress. Modern research increasingly shows that these disorders involve complex dysfunction within autonomic regulatory networks rather than simply isolated cardiovascular abnormalities. (pmc.ncbi.nlm.nih.gov)
What Happens During a Tilt Table Test?
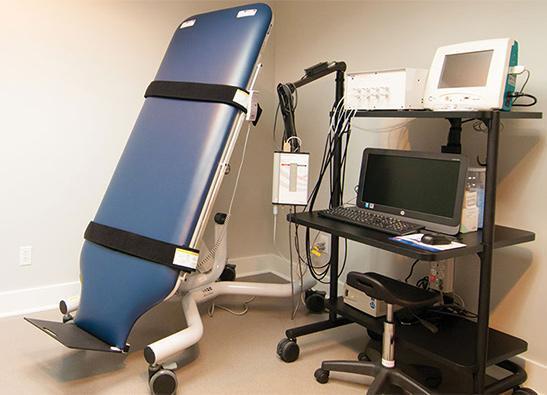
During the procedure, a patient lies securely strapped to a motorized table while clinicians continuously monitor:
- Heart rate
- Blood pressure
- Electrocardiogram (ECG) activity
- Oxygen levels
The table is then gradually tilted upward to simulate standing while the patient remains supported. This allows physicians to observe how the autonomic nervous system reacts to orthostatic changes — the physiological stress caused by gravity when standing upright. (mayoclinic.org)
In healthy individuals, standing triggers rapid autonomic reflexes that maintain blood flow to the brain. Blood vessels constrict, heart rate adjusts slightly, and blood pressure stabilizes almost immediately. In autonomic disorders, these responses may become delayed, exaggerated, or insufficient.
How Tilt Table Testing Helps Diagnose POTS
One of the most common reasons for tilt table testing is evaluating suspected postural orthostatic tachycardia syndrome (POTS).
POTS is a form of autonomic dysfunction characterized by an excessive increase in heart rate when standing without a major drop in blood pressure. Patients may experience:
- Dizziness
- Brain fog
- Fatigue
- Heart palpitations
- Lightheadedness
- Exercise intolerance
- Nausea
- Syncope or near-fainting episodes
According to the 2022 clinical review Diagnosis and Management of Postural Orthostatic Tachycardia Syndrome (POTS), the condition involves abnormal autonomic regulation, altered sympathetic nervous system activity, impaired vascular tone, and dysfunction in orthostatic adaptation pathways. (pmc.ncbi.nlm.nih.gov)
Tilt table testing allows clinicians to objectively measure these abnormal responses and determine whether autonomic instability is contributing to symptoms.
Orthostatic Hypotension and Dysautonomia
Tilt table testing is also frequently used to diagnose orthostatic hypotension — a condition in which blood pressure drops excessively upon standing. Symptoms often include:
- Blurred vision
- Weakness
- Dizziness
- Fatigue
- Fainting
In many cases, the autonomic nervous system fails to adequately constrict blood vessels against gravity, leading to reduced cerebral blood flow and impaired circulation to the brain.
Dysautonomia is a broader term that refers to disorders affecting autonomic nervous system regulation. Tilt table testing helps physicians evaluate how well autonomic reflexes maintain cardiovascular stability during positional changes.
What Does the Tilt Table Test Reveal About the Nervous System?
Beyond measuring heart rate and blood pressure, tilt table testing offers insight into how the brainstem and autonomic nervous system process gravitational information.
Specialized graviceptive fibers within the vestibular system detect head position and movement relative to gravity. These signals travel through vestibular nuclei in the brainstem and interact with autonomic control centers responsible for regulating blood pressure and heart rate during posture changes. (pmc.ncbi.nlm.nih.gov)
When functioning properly, these vestibular-autonomic pathways rapidly activate compensatory reflexes that maintain cerebral perfusion while standing. In dysautonomia and POTS, researchers believe these pathways may become dysregulated, resulting in abnormal autonomic signaling, altered baroreflex responses, and impaired cardiovascular adaptation to gravity.
Emerging research suggests that autonomic dysfunction may involve both peripheral nervous system abnormalities and dysfunction within central autonomic processing networks in the brainstem. (arxiv.org)
Common Treatments After a Tilt Table Test
After diagnosing autonomic dysfunction, physicians often recommend strategies that improve orthostatic tolerance and symptom management.
Increased Salt and Fluid Intake
Higher sodium and fluid intake may help expand blood volume and improve circulation to the brain. This is one of the most commonly recommended interventions for POTS patients. (pmc.ncbi.nlm.nih.gov)
Compression Socks and Compression Garments
Compression socks and abdominal binders help reduce blood pooling in the lower extremities during standing, improving venous return and reducing dizziness.
Physical Therapy and Graded Exercise
Physical therapy programs often focus on:
- Recumbent exercise
- Lower-extremity strengthening
- Vestibular rehabilitation
- Cardiovascular conditioning
- Autonomic retraining
These approaches may improve orthostatic tolerance over time.
Medication Management
Depending on the diagnosis, medications may be prescribed to:
- Increase vascular tone
- Expand blood volume
- Regulate heart rate
- Support autonomic stability
Lifestyle Modifications
Additional recommendations often include:
- Avoiding prolonged standing
- Rising slowly from seated positions
- Improving sleep quality
- Staying hydrated
- Reducing overheating
- Managing nervous system stress
Do Current Treatments Solve the Underlying Problem?
While many patients experience improvement with salt loading, compression therapy, medications, and exercise programs, these treatments often focus on symptom management rather than correcting the underlying autonomic dysfunction itself.
The 2022 review Diagnosis and Management of Postural Orthostatic Tachycardia Syndrome (POTS) emphasizes that current therapies primarily aim to improve functional capacity and orthostatic tolerance. However, many researchers now believe that deeper dysfunction within autonomic neural networks, baroreflex pathways, vestibular-autonomic integration systems, and brainstem regulation may contribute to the root cause of these conditions. (pmc.ncbi.nlm.nih.gov)
This is why ongoing research into neuroplasticity, autonomic rehabilitation, vestibular pathways, neuroinflammation, and central nervous system regulation is becoming increasingly important in dysautonomia care.
Research Articles on Tilt Table Testing and Autonomic Stability
1. Diagnosis and Management of Postural Orthostatic Tachycardia Syndrome (POTS) — 2022
Diagnosis and Management of Postural Orthostatic Tachycardia Syndrome (POTS)
A comprehensive modern review discussing:
- POTS diagnosis
- Tilt table testing
- Autonomic dysfunction
- Orthostatic intolerance
- Current treatment strategies
2. Tilt Test: A Review — 2021
An in-depth review of tilt table physiology, cerebral blood flow regulation, autonomic reflexes, and orthostatic stress responses.
3. Characterization of Blood Pressure and Heart Rate Oscillations in POTS Patients
Characterization of Blood Pressure and Heart Rate Oscillations in POTS Patients
Research examining abnormal cardiovascular oscillations, autonomic instability, and baroreflex dysfunction during tilt table testing in POTS patients.
Final Thoughts
A tilt table test is far more than a simple fainting evaluation. It provides clinicians with valuable insight into how the autonomic nervous system, cardiovascular system, vestibular pathways, and brainstem interact to regulate blood pressure and circulation during orthostatic stress.
For patients struggling with dizziness, rapid heart rate, chronic fatigue, fainting, or dysautonomia symptoms, tilt table testing can uncover patterns of autonomic dysfunction that may otherwise go undetected. While current treatments often help improve quality of life and symptom control, modern research suggests that many autonomic disorders involve deeper dysfunction within the nervous system itself — highlighting the need for continued advances in autonomic rehabilitation and neurological treatment approaches.
Forrest Fisher
Contact Me